Realities of life on GLP-1s for weight loss
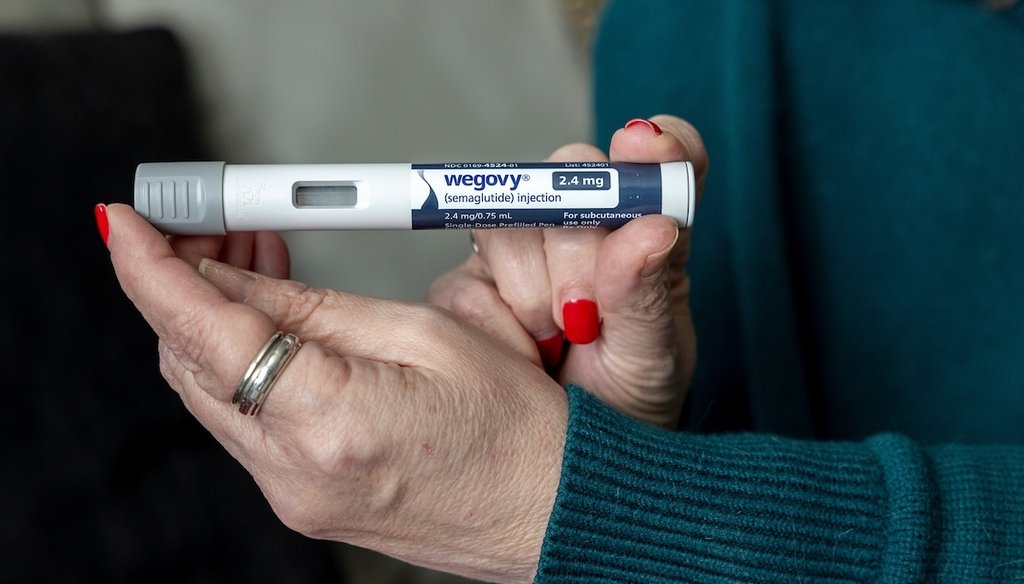
GLP-1s are everywhere. They’re featured in ads, celebrity headlines, friends’ anecdotes and endless online takes. Yet clarity about what it’s like to actually take these medications is in short supply. Are they a miracle weight-loss drug, or riddled with side effects?
We wanted to better understand what life on GLP-1s for weight loss really looks like: What can you expect when you first start taking the drug? What lifestyle changes do doctors advise? What happens if you stop?
We spoke with three doctors who specialize in weight loss and prescribe these medications. We learned that although the drugs may provide a fast-lane to weight loss, diet and exercise remain key to avoid malnutrition, minimize side effects, and keep your bones and muscles strong.
What are GLP-1s?
GLP-1 stands for glucagon-like peptide-1.
GLP-1 agonists are a whole class of drugs with various generic and brand names — semaglutide (Ozempic/Wegovy/Rybelsus), dulaglutide (Trulicity), exenatide (Byetta), liraglutide (Saxenda/Victoza) and tirzepatide (Mounjaro/Zepbound) to name a few.
Most are injected – sometimes weekly, sometimes daily — but some can be taken as a pill.
U.S. drug regulators first approved GLP-1s in 2005 to treat Type II diabetes. Liraglutide (Saxenda) earned FDA approval in 2014 to treat weight loss, but GLP-1s as a class took off with the 2021 approval of semaglutide (Wegovy) for chronic weight management.
By the fall of 2025, one in eight American adults were taking a GLP-1 drug, a KFF poll found.
These medications regulate blood sugar and reduce appetite, which can lead to significant weight loss. Studies of GLP-1s show patients’ average weight loss ranges from 5% to 20% of their body weight. The drugs also show benefits for other health issues such as sleep apnea, cardiovascular disease and arthritis.
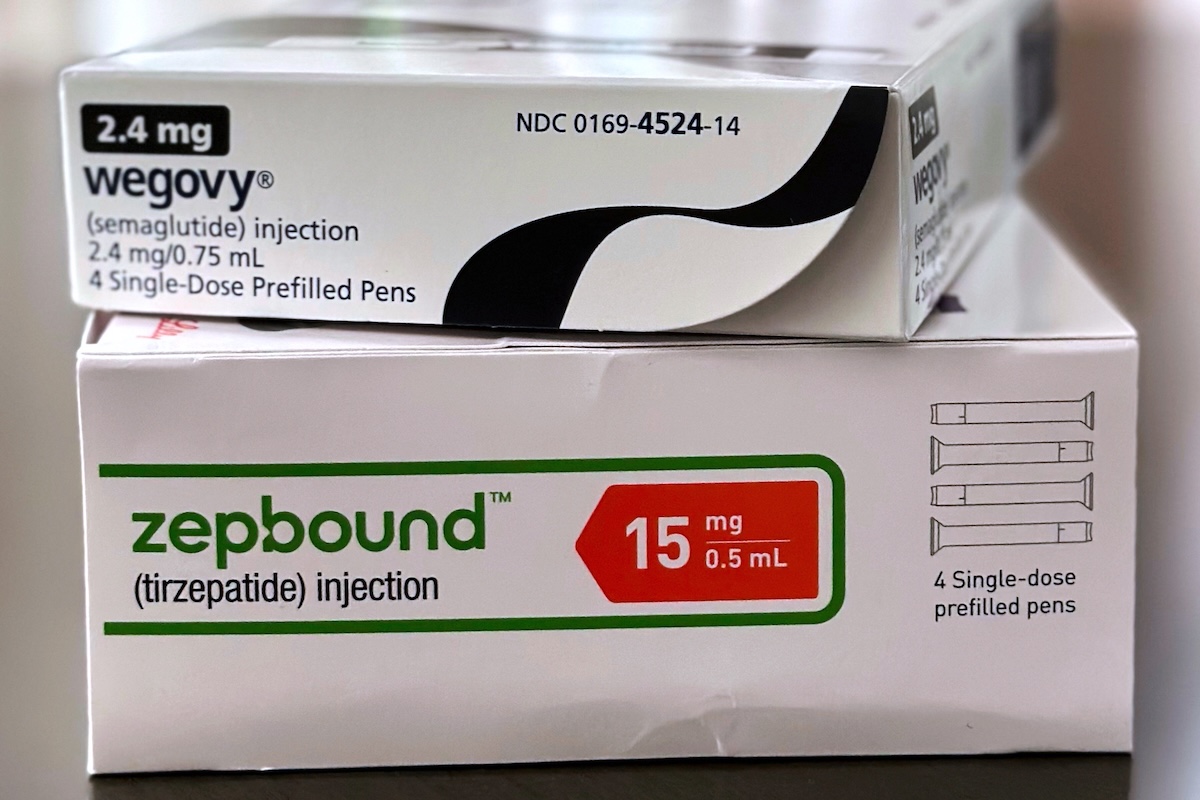
Boxes for the GLP-1 medications Wegovy (semaglutide) and Zepbound (tirzepatide) pictured in California, May 8, 2025. GLP-1s as a class took off when semaglutide was approved for chronic weight management in 2021. (AP)
What to expect when starting a GLP-1
Patients who start GLP-1s for weight loss may first notice they feel more full after eating and think less about food, sometimes called “food noise.”
Nausea, vomiting, bloating, diarrhea and constipation are normal in these first few days and after a dosage increase. During this period, patients may find it best to opt out of late-night activities and intense workouts.
Dr. Robert F. Kushner, an obesity medicine specialist and Northwestern University professor emeritus, recommends eating slowly, in smaller portions, and avoiding fatty or greasy foods that may cause bellyaches. And although the drugs reduce hunger, patients on GLP-1s should still eat three meals a day and stay hydrated.
The good news is that the body can get used to the medication. The typical treatment requires starting at a low dose and gradually increasing it every four weeks.
“I think people think, ‘Well, I’m on this low dose, if I feel this bad on the low dose, I’m going to feel terrible on the higher dose,’” said Dr. Daniel Bessesen, chief endocrinologist at the University of Colorado School of Medicine. But patients’ side effects can decrease over time as their dosage stabilizes, he said.
Bessesen said if patients experience bad side effects, lose weight too rapidly or see good progress on a lower dose, they can talk to their doctors about staying on a lower dose longer.
Rare side effects linked to GLP-1 medications include pancreatic inflammation, acute kidney damage and gallbladder issues.

A modified menu catering to the dietary needs of people who use GLP-1 weight loss drugs is displayed at Cuba Libre Restaurant and Rum Bar in Philadelphia, on Friday, March 6, 2026. (AP)
Lifestyle changes to diet and exercise on the medications
So you got on a GLP-1. Now what? Diet and exercise are key.
Dr. Scott Kahan, an obesity medicine specialist in Washington, D.C., said it’s very important that patients continue to get enough calories, even though the medication will make them feel less hungry.
“Losing too much weight or losing too quickly is counterproductive and may be dangerous,” he said.
Getting too few calories can lead a person to become deficient in protein, calcium and iron — nutrients the body needs to function.
Losing weight too fast can also harm bone and muscle health. Losing some bone and muscle mass is inevitable any time a person loses significant weight. But losing the weight too rapidly can exacerbate the damage — the body will not only break down fat stores for energy (the goal of weight-loss), but start to break down muscle tissue as well.
To lose weight at a more moderate pace (1-2 pounds a week) and ensure adequate nutrition, here’s what doctors advise.
-
Plan out meals in advance. Think about the week ahead — where’ll you be at mealtimes and what’ll you’ll eat. And don’t skip meals, even if you don’t feel hungry — even a protein bar and yogurt at lunch is better than nothing. Going long periods without eating may lead to worse side effects like nausea.
-
Eat nutritionally dense foods. Because your calorie intake is likely to drop, the ones you do eat should be nutrient-packed. Think fruits and vegetables, lean proteins and whole grains.
-
Get lots of protein and fiber. Sufficient protein intake — at least 1/2 gram per pound of body weight a day — can help protect the body from bone and muscle mass loss. Fiber is also important to keep gastrointestinal side effects like constipation and diarrhea at bay.
-
Exercise to maintain bone and muscle strength. Both cardio and strength and resistance training help mitigate bone and muscle mass loss. Kusher said exercising twice a week is ideal. Certain populations such as seniors and post-menopausal women who are already at risk of bone loss should discuss their bone health with their doctor before taking these medications.
Bessesen said patients should also understand the effect these medications can have on their social life. Holiday meals, happy hours and standing Taco Tuesdays may lead to new conversations. Who do you want to know you are taking the medication? How might you respond to social pressure to eat when you’re not hungry?

Donna Cooper shows her exercise bike at her home in Front Royal, Virginia, on March 1, 2024. Cooper was taking Wegovy when she told The Associated Press that she maintained her fitness regimen with walks with friends. She hoped to continue with a strict diet and exercise plan after she finished taking the drug. (AP)
To stop or not?
Although these medications are often advertised as a short-term strategy, that’s not how doctors see them.
“I tell people they should be prepared to take the medicine long term,” Bessesen said, comparing it with a blood pressure or cholesterol medication.
The benefits of these medications appear to last only as long as you are on them. It’s not true for everyone, but people who stop the medication typically regain much of the weight they lost.
It’s not about willpower, but the biologic need to eat Kushner said. People might adhere to certain diet and exercise habits while they are taking the drug, but hunger and food noise returns once they stop. It’s like asking you to “stop breathing, hold your breath for two minutes,” Kushner said. “Why can’t you? Well, because I can’t.”
With 20 years of data on using GLP-1s to treat diabetes, scientists haven’t identified any significant long-term complications, Kushner said.
Bessesen said most of his patients want to come off the medication after the weight is lost. Statistics show that most people quit within the first year. Patients who take this route should consult with their doctors about post-GLP-1 weight management strategies.
It may be easy to access GLP-1s online, but doctors don’t recommend going it alone without a doctor’s input. A doctor can help you consider these treatments within the context of your overall health goals and history.
“This is a big deal,” Bessesen said.